You've tried to build better routines. Tried to wind down at night. Tried to start the morning differently. And every time, something in your body seems to override your intentions, like a restless evening, brain fog that kills your momentum, or a wave of tension that pulls you off track.
What if the problem isn't only in your head? Researchers are learning that your gut and your brain are in constant two-way conversation, and that conversation may shape how you feel and how easily routines stick.
Consider this: roughly 90% of your body's serotonin is produced in your gut — not your brain. That's established neuroscience. The enteric nervous system — a network of over 500 million neurons lining your gastrointestinal tract — is so complex that researchers call it "the second brain." And it doesn't just digest your food. Research suggests it may play a role in mood, the stress response, and how steady you feel day to day.*
The Highway Between Your Gut and Your Brain
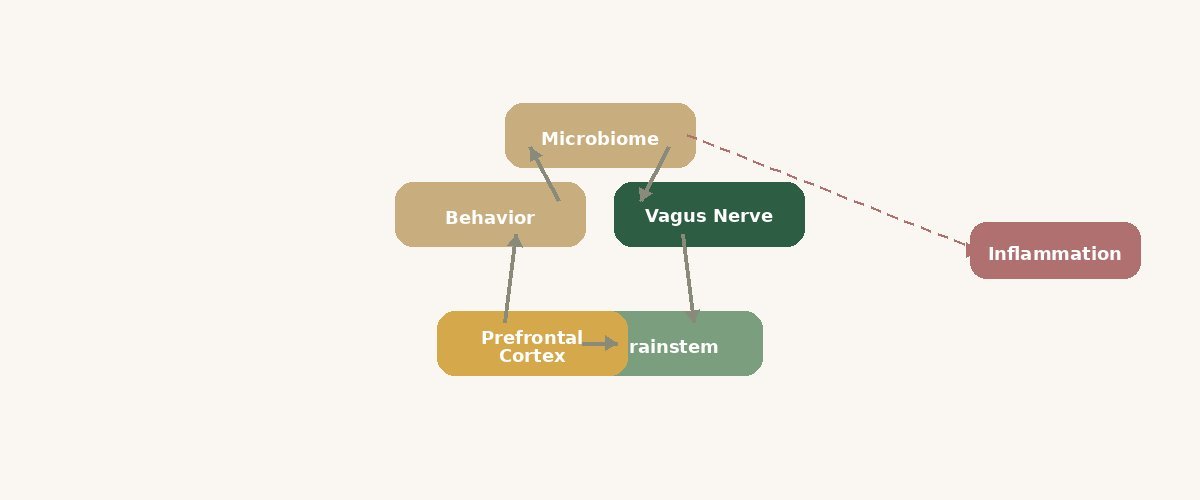
The vagus nerve — the same nerve we talk about in nervous system regulation — is the primary communication channel between your gut and your brain. And here's what most people miss: an estimated 80% of the signals traveling through the vagus nerve go from the gut up to the brain. Not the other way around.*
Your gut is not just receiving instructions. It is part of a two-way signal loop with your brain. Researchers are exploring how this communication may relate to mood, stress, and how supported you feel when you try to change a routine.*
This is the gut-brain axis, and understanding it changes everything about how you approach behavior change.
The Community of Microbes in Your Gut
Your gut hosts trillions of microorganisms. Researchers have found that some of the same chemical messengers your brain uses, such as serotonin and dopamine, are also linked to activity in the gut. Science is still working out what this means for behavior.*
What you eat, how you sleep, and how stressed you are can all be part of this picture. Better Life Habits does not teach diet plans or food targets, and questions about food are best worked out with a qualified professional. What we focus on is the part of the system you can support with simple daily routines.
When a habit falls apart under stress, it is not just weak willpower. Your body and its internal state are part of the equation. Understanding that isn't an excuse, it's a reason to start with the body instead of fighting yourself.
The encouraging part is that this is not fixed. Your internal state can shift as you change your daily routine. You are not stuck with how you feel today.
Stress, the Body, and Why Habits Wobble
When you are under sustained stress, your body shifts into a state that prioritizes alertness over rest and recovery. Many people notice that digestion, sleep, and steadiness all feel off during these stretches.
This matters for habits because the part of the brain involved in planning and follow-through, the prefrontal cortex, tends to work best when your body feels safe and rested, not when it is braced and depleted.*
It can become a loop: stress makes follow-through harder, which leads to choices you would not make when rested, which adds more stress. If your habits seem to fall apart during your hardest stretches, this is part of why, and it is not a character flaw.*
Research on the autonomic nervous system fits this picture: when the body is in a prolonged fight-or-flight state, it diverts energy away from rest-and-digest functions. Your nervous system state and your gut appear to influence each other.*
What This Means for Building Habits
If you're trying to build new habits while your body is running on stress and little recovery, you're working against a headwind that no amount of motivation fully overcomes.*
This is why we start with the body at Better Life Habits. It's not a warm-up, it's the foundation. When your nervous system settles, the parts of you involved in planning and follow-through tend to come back online. Then change gets easier, not through force, but because the conditions support it.*
Three research-informed entry points:
Support your nervous system first. Breathing practices, calming techniques, and gentle stress-release routines (all in the Calm Start Kit) may help your body shift out of a constant fight-or-flight state. Start here, and other things often feel easier to follow.*
Start with your nervous system. The gut often follows. The free Calm Start Kit includes calming practices that may support gut-brain communication — or get The Calm Sleep Reset for the complete routine.
Move and get daylight. Gentle movement and some morning light are simple, body-first ways to support a steadier daily rhythm. They ask nothing of your willpower, and they help set the cues your body uses to feel settled. A short walk counts.*
Protect your sleep. Sleep is when your body does much of its recovery, and short or broken sleep makes almost everything harder the next day, including follow-through. Even small, consistent improvements to your wind-down can help. Sleep is not separate from how steady you feel, it is part of the same system.*
Your body is not working against you. It is responding to its conditions. Working with that, instead of fighting it, is the difference between habits that collapse under pressure and habits that hold. Biology, not belief.
The Bigger Picture
The gut-brain connection is one of the most active areas of research right now, and it is still developing. It links systems we used to think of as separate, like mood, sleep, and behavior. Seeing them as connected changes how you approach habit change.*
You stop asking "why can't I stick with this?" and start asking "what biological state am I in when I try?" That question leads to different strategies, different interventions, and different results.
This is what we mean by biology over belief. Your body isn't working against you. It's responding to conditions. Change the conditions, and the behavior follows.
Start With Your Nervous System.
The Calm Start Kit gives you 7 free body-first practices to help your nervous system settle. Or get the full 7-day sleep-support routine.
Sources & Further Reading
- Cryan, J. F. & Dinan, T. G. (2012). Mind-altering microorganisms: The impact of the gut microbiota on brain and behaviour. Nature Reviews Neuroscience, 13(10), 701–712.
- Mayer, E. A. (2016). The Mind-Gut Connection. Harper Wave.
- Carabotti, M. et al. (2015). The gut-brain axis: Interactions between enteric microbiota, central and enteric nervous systems. Annals of Gastroenterology, 28(2), 203–209.
- Yano, J. M. et al. (2015). Indigenous bacteria from the gut microbiota regulate host serotonin biosynthesis. Cell, 161(2), 264–276.
*Educational content only. Not medical, psychological, or therapeutic advice. Routines shared for informational purposes. Consult healthcare professionals before making health changes. Individual results vary. References to research are for educational context; Better Life Habits does not claim clinical validation of its specific protocols.
