You're exhausted. You've been tired all day. You finally sit down, finally close your eyes, and your brain lights up like a fire alarm. Thoughts racing, shoulders tense, heart rate won't settle. You're too tired to do anything, and too wired to rest.
This state has a name. Researchers call it sympathetic dominance. You probably call it "tired but wired." And it isn't a character flaw or a mindset problem. It's a specific biological state where your nervous system has lost the ability to downshift on its own.*
What "Tired But Wired" Actually Is
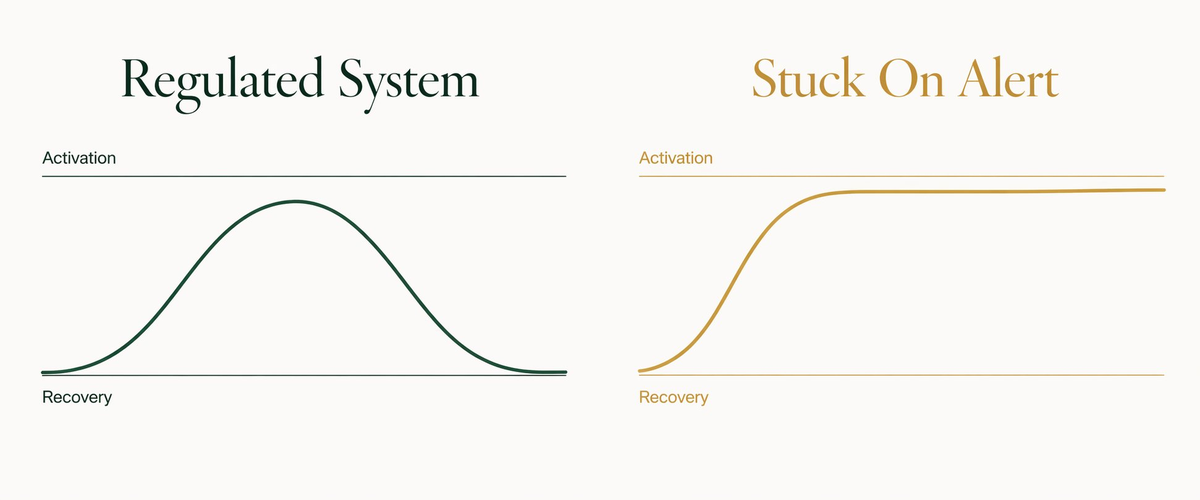
Your autonomic nervous system has two major branches. Sympathetic, often called fight-or-flight, ramps up the body to handle threat, effort, or urgency. Parasympathetic, often called rest-and-digest, brings the body down into recovery, digestion, and sleep. A healthy system toggles between these fluidly all day long.*
Tired-but-wired is what happens when the sympathetic branch gets stuck in the "on" position. Cortisol and adrenaline stay circulating. Heart rate variability drops. Muscle tone stays high. You feel the exhaustion because the body has been in high-output mode for too long, and you feel the wiring because the off switch isn't working.*
Four biological patterns keep this loop running. Fix these, and the system regains its ability to downshift.
Reason 1: Your Cortisol Curve Is Reversed
Cortisol should peak in the morning and fall through the day, hitting its lowest point at night. Under chronic stress, that curve flattens or flips. You end up running on empty in the morning and surging at 10PM, right when the body should be winding down.*
When cortisol is still high at bedtime, your nervous system doesn't get the hormonal signal to switch branches. You lie in bed with a tired body and a revved-up brain because the hormone that would normally quiet the system isn't quieting.*
Reason 2: Your Breathing Has Shifted
Most people under chronic stress start breathing in a pattern that locks the sympathetic branch on. Shallow, fast, upper-chest breaths. Inhale-dominant. Rarely a full exhale.*
This matters because the single fastest way to activate the parasympathetic branch is through a long, slow exhale. The vagus nerve is stimulated mechanically on the exhale. If you're not exhaling fully, you're starving the system of its primary downshift signal — all day, every day, without realizing it.*
Reason 3: Sensory Overload and Hypervigilance
Notifications, background noise, constant task-switching, open browser tabs, overhead fluorescent light. Each is a small activation signal to the nervous system. Individually they're nothing. Stacked, they keep the brain in low-grade threat assessment mode for hours at a time.*
Over weeks and months, this trains hypervigilance into the baseline. The nervous system stops distinguishing between actual threat and environmental noise. Everything registers as "stay alert." By evening, the system literally doesn't know how to come down because it hasn't been given a clear "safe" signal in hours.*
Reason 4: The Gut-Brain Stress Loop
The vagus nerve runs between your gut and your brain, and roughly 80% of its fibers carry information from the gut upward. When gut inflammation is elevated — often caused by chronic stress itself — the vagus sends continuous alarm signals to the brain, which reads them as threat and keeps the sympathetic branch active.*
This is why poor gut health and a stuck nervous system usually travel together. The body can't settle into rest because one of its biggest communication channels is telling the brain something is still wrong.*
Tired-but-wired isn't a willpower failure. It's four biological patterns running in parallel. Interrupt any one of them and the system starts to move again.
How to Exit the Loop
The fastest way out is to give the nervous system direct, mechanical signals that it's safe to downshift. Not affirmations. Not positive thinking. Physical inputs the body can't ignore.*
Extended exhales. Inhale for 4 counts, exhale for 6 to 8. Five to ten rounds. This is a manual override for the parasympathetic branch.*
Cold water on the face or wrists. Activates the diving reflex, which triggers an immediate vagal response and slows heart rate.*
Humming or slow vocalization. The vagus nerve passes through the vocal cords; humming produces mechanical vibration that stimulates it directly.*
Bilateral slow movement. Walking outside at an easy pace signals the brain that you are not under threat. Ten minutes is usually enough to shift state.*
Want all four protocols in one place? The free Calm Start Kit gives you three nervous system regulation tools you can use tonight, including the 2-Minute Downshift Reset. Or get The Calm Sleep Reset for the complete 7-day protocol.
The goal isn't to get rid of the sympathetic branch. You need it. The goal is to rebuild the bridge between activation and recovery so the system can move through both instead of getting stuck in one. Most people feel a shift within the first week of consistent practice. Biology, not belief.*
Work With Your Biology Instead of Against It.
The Calm Sleep Reset is a complete 7-day protocol built on behavioral sleep science. Start with the free Calm Start Kit tonight, or go deeper with the full reset.
Sources & Further Reading
- Porges, S. W. (2007). The polyvagal perspective. Biological Psychology, 74(2), 116–143.
- McEwen, B. S. (2007). Physiology and neurobiology of stress and adaptation: Central role of the brain. Physiological Reviews, 87(3), 873–904.
- Ma, X., Yue, Z. Q., Gong, Z. Q., Zhang, H., Duan, N. Y., Shi, Y. T., Wei, G. X., & Li, Y. F. (2017). The effect of diaphragmatic breathing on attention, negative affect and stress in healthy adults. Frontiers in Psychology, 8, 874.
- Arnsten, A. F. T. (2009). Stress signalling pathways that impair prefrontal cortex structure and function. Nature Reviews Neuroscience, 10(6), 410–422.
*Educational content only. Not medical, psychological, or therapeutic advice. Protocols shared for informational purposes. Consult healthcare professionals before making health changes. Individual results vary. References to research are for educational context; Better Life Habits does not claim clinical validation of its specific protocols.
