You keep waiting to feel like yourself again. You take the weekend off. You go on vacation. You do the meditation, the yoga, the journaling. And still, underneath all of it, something in your body is braced for impact.
That isn't stress. Stress is episodic. This is something else. When your nervous system has been running the same threat response for months or years, the response stops being a reaction and starts being a baseline. Researchers call it allostatic load. You probably call it survival mode. And exiting it requires something more specific than "relaxing more."*
Survival Mode Is a Biological State, Not a Mindset
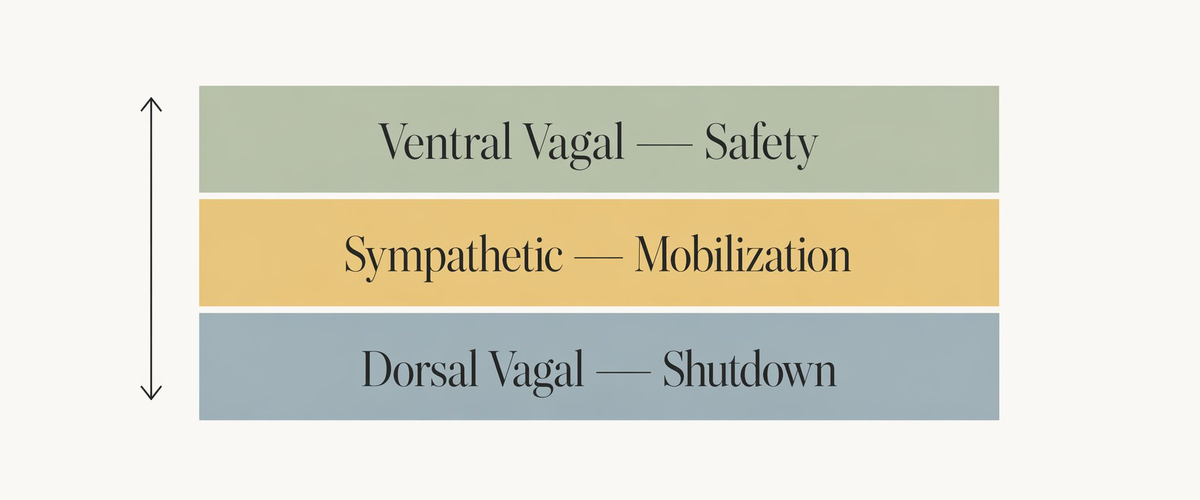
Stephen Porges' polyvagal theory describes the nervous system as operating in three primary states. Ventral vagal is the state of safety, connection, and regulated function — where rest, digestion, and clear thinking happen. Sympathetic is the state of mobilization, where the body prepares for fight or flight. Dorsal vagal is a shutdown state, where the system essentially powers down to conserve resources when threat feels inescapable.*
Survival mode is what happens when the system loses fluid access to ventral vagal and gets stuck bouncing between sympathetic activation and dorsal shutdown. The body is either running hot or running flat, rarely both online at the same time, and the internal signal that would tell it "you're safe now" has gone quiet.*
Four signs show up consistently when this state has become chronic.
Sign 1: Rest Doesn't Feel Restful
You sit down. You try to relax. Within minutes, you're up doing something else — checking your phone, scanning the room, reorganizing a drawer. It's not a discipline problem. It's a nervous system problem.*
When the system is stuck in sympathetic, inactivity registers as vulnerability. The body doesn't interpret stillness as rest; it interprets stillness as exposure. So the system keeps generating small activations to stay alert. Real rest requires a baseline perception of safety, and if that baseline has been offline for too long, even sitting on a couch can feel like something to escape.*
Sign 2: Small Decisions Feel Overwhelming
You stand in front of the pantry unable to pick what to eat. An email takes 45 minutes to answer. A normal weekend plan feels like too much to coordinate. This isn't laziness or depression on its own — it's a specific consequence of prolonged cortisol elevation on the prefrontal cortex.*
Research on chronic stress has shown measurable impairment in prefrontal function under sustained cortisol load. Working memory narrows. Decision-making slows. The brain essentially reverts to simpler, habit-driven responses because the cognitive capacity for novel choice has been drained by the ongoing threat response.*
Sign 3: Your Body Is Always Braced
Jaw clenched. Shoulders up by your ears. Shallow breath sitting high in the chest. Tension in the belly you don't notice until you lie down. The body of someone in chronic survival mode looks like it's preparing for something.*
Muscular bracing is an automatic sympathetic output. Under acute stress, it prepares the body to move, strike, or flee. Under chronic stress, it becomes the default posture even when nothing is happening. The body forgets how to let go because letting go has stopped being associated with safety.*
Sign 4: Sleep Is Broken Even When You're Exhausted
You fall asleep fast from pure depletion. You wake at 2 or 3AM and can't get back down. You sleep 7 hours and feel like you slept 3. The tiredness never fully clears.*
This pattern is the sleep signature of a nervous system that can't access parasympathetic dominance long enough for restorative sleep. Deep sleep and REM both require a fully downshifted system. When the system is stuck sympathetic, sleep happens mostly in the lighter stages, which produces hours in bed but very little actual recovery.*
Survival mode doesn't end because you realize you're in it. It ends because you give the nervous system enough consistent safety signals that it finally believes it can stand down.
How to Exit Survival Mode
Exiting requires two things at once: interrupting the active threat response, and rebuilding the baseline perception of safety. Neither happens through insight alone. Both happen through specific, repeatable physical inputs.*
Daily vagal tone practice. Long exhales, humming, cold water to the face. Three to five minutes, at least twice a day. You're not trying to solve anything. You're training the system's ability to downshift on command.*
Predictable daily anchors. Same wake time. Same meal times. Same wind-down sequence. A nervous system in survival mode calms faster in a predictable environment because predictability is itself a safety signal.*
Co-regulation with a safe other. Porges' research shows that the fastest way to shift a dysregulated system is proximity to a regulated one. A calm conversation with someone you trust, a walk with a steady friend, time with a pet. These aren't fluff; they're biological interventions.*
Gentle, rhythmic movement. Walking outside. Slow stretching. Not high-intensity exercise, which can push a sympathetic system further into activation. Rhythmic, bilateral, low-effort movement signals the brain that you're not in acute threat.*
Protected sleep. Phone out of bedroom, consistent wake time, dim lights in the evening. Sleep is where the system does its deepest repair, and survival mode will not truly resolve if sleep stays broken.*
Ready to step out of survival mode? The free Calm Start Kit includes three nervous system regulation protocols designed to interrupt sympathetic dominance. Or get The Calm Sleep Reset for the complete 7-day protocol.
Getting out of survival mode is a nervous system project, not a willpower project. It takes weeks, not days. But the system is built to return to regulation when given the right signals consistently. Your body isn't broken. It's waiting for proof that it's safe to stand down. Biology, not belief.*
Work With Your Biology Instead of Against It.
The Calm Sleep Reset is a complete 7-day protocol built on behavioral sleep science. Start with the free Calm Start Kit tonight, or go deeper with the full reset.
Sources & Further Reading
- Porges, S. W. (2011). The Polyvagal Theory: Neurophysiological Foundations of Emotions, Attachment, Communication, and Self-regulation. W. W. Norton.
- McEwen, B. S. (2007). Physiology and neurobiology of stress and adaptation: Central role of the brain. Physiological Reviews, 87(3), 873–904.
- Arnsten, A. F. T. (2009). Stress signalling pathways that impair prefrontal cortex structure and function. Nature Reviews Neuroscience, 10(6), 410–422.
- van der Kolk, B. A. (2014). The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma. Viking.
*Educational content only. Not medical, psychological, or therapeutic advice. Protocols shared for informational purposes. Consult healthcare professionals before making health changes. Individual results vary. References to research are for educational context; Better Life Habits does not claim clinical validation of its specific protocols.
