You fell asleep fine. Maybe even quickly. Then at 3AM your eyes snap open, your mind starts looping, and you lie there for the next hour trying to will yourself back to sleep. Sound familiar?
This pattern is so common that most people assume it's insomnia. It's not. For the vast majority of people who wake between 2 and 4AM, the cause is biological and specific, and it has a name: a dysregulated cortisol curve.*
It's Not Insomnia. It's Cortisol.
Cortisol is your body's primary stress and wake-up hormone. In a regulated nervous system, cortisol follows a predictable daily rhythm called the diurnal curve. It surges in the early morning to wake you up, peaks about 30 minutes after you open your eyes, then falls steadily through the day until it bottoms out late at night so you can sleep.*
The 3AM wake-up happens when that curve gets scrambled. Instead of staying low through the night, cortisol starts climbing too early, too hard. Your brain interprets the surge as "time to be awake," even though your body is nowhere near done sleeping.*
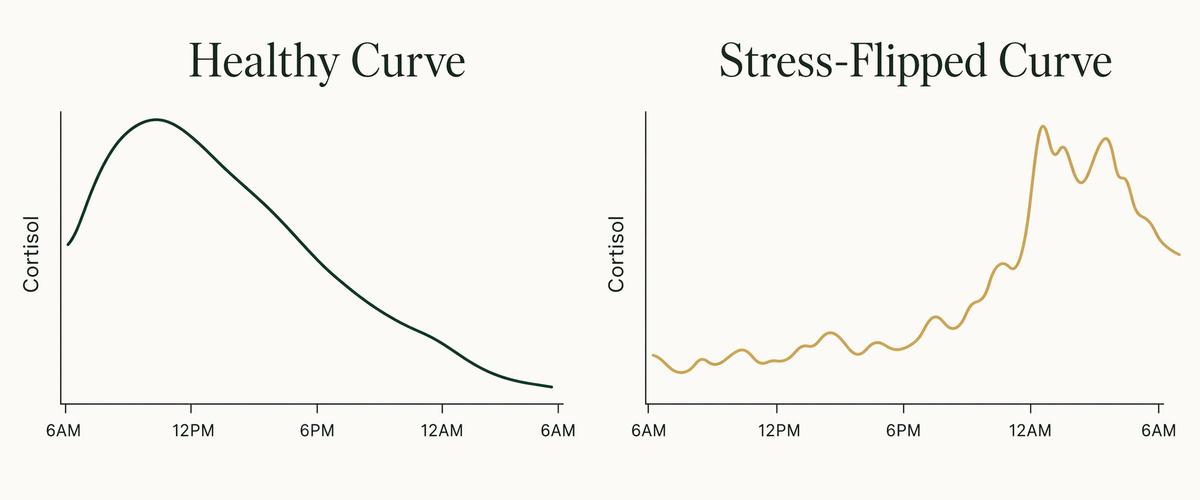
Your Body's Normal Cortisol Curve
Under healthy conditions, cortisol at 3AM should be near its lowest point of the entire 24-hour cycle. This is when growth hormone does repair work, the glymphatic system clears brain waste, and REM sleep consolidates memory. All of that requires cortisol to stay quiet.*
The first real cortisol rise is supposed to happen between 4 and 6AM, gradually, as your body prepares for the transition to wakefulness. That's the foundation of what researchers call the Cortisol Awakening Response (CAR) — a sharp spike that peaks roughly 30 minutes after you open your eyes and gives you the alertness to start your day.*
Why Chronic Stress Flips the Curve
Chronic stress doesn't just raise cortisol. It rearranges when cortisol fires. Long-term activation of the HPA axis — the stress response system that controls cortisol release — progressively disrupts the timing of the whole cycle.*
Research on diurnal cortisol slopes has found that people under chronic stress often show a flatter curve, a reversed curve (high at night, low in the morning), or an abnormally early cortisol rise in the middle of the night. These patterns are associated with worse sleep quality, impaired immune function, and higher rates of mood disorders.*
The practical translation: if you've been under stress for months or years, your body may no longer know what time of day it is at a hormonal level. Cortisol fires when it shouldn't. Sleep breaks when it used to hold.*
The 3AM Pattern, Explained
Here's what's likely happening on a typical 3AM wake-up:
Between 2 and 4AM, your body begins its natural cortisol rise to prepare for waking hours later. In a regulated system, that rise is gentle and doesn't disturb sleep. In a dysregulated system, it comes on too strong, too fast. Your brain receives the cortisol signal and shifts out of deep sleep into a lighter stage. That alone isn't enough to wake you — but now your nervous system is already elevated, which means any small stimulus (a sound, a thought, a full bladder) becomes the thing that tips you into full alertness.*
Once you're awake, the racing mind follows. Cortisol primes the brain for threat scanning. Your thoughts go immediately to work deadlines, finances, health, whatever stressor is closest. You try to calm down. The effort itself releases more cortisol. The loop gets tighter.*
3AM waking is your nervous system firing a wake signal at the wrong time. The fix isn't trying harder to fall back asleep. It's retraining the system so the wake signal stops firing in the first place.
How to Break the 3AM Cycle
Breaking the pattern isn't about what you do at 3AM. It's about what you do in the 24 hours before. A handful of behavioral protocols consistently show up in the research on cortisol regulation:*
Morning light within an hour of waking. Direct outdoor light in the first hour after rising is the strongest known signal for setting your circadian clock. It anchors the cortisol curve so it peaks in the morning, not the middle of the night.*
Consistent sleep and wake times. Your HPA axis entrains to a schedule. Irregular bedtimes keep it guessing, which keeps cortisol firing unpredictably.*
Long, slow exhales before bed. Extended exhalation activates the vagus nerve and downshifts the nervous system into parasympathetic dominance. A few rounds of 4-count inhale, 6 to 8-count exhale, 5 minutes before lights out, is enough to measurably lower pre-sleep cortisol.*
Phone out of the bedroom. The blue light and the dopamine hit of late-night scrolling both elevate cortisol. Charge the phone in another room and use a cheap alarm clock instead.*
A designed 3AM response. If you do wake up, the worst thing is lying there fighting it. Having a pre-planned protocol — slow breathing, body scan, getting out of bed briefly if needed — interrupts the panic loop and prevents the cortisol spike from compounding.*
Done lying awake at 3AM? The free Calm Start Kit includes the 3AM Rescue Plan — a step-by-step protocol for falling back asleep when you wake up stuck. Or get The Calm Sleep Reset for the complete 7-day protocol.
The 3AM wake is your body telling you something specific: the cortisol curve is off. You don't fix it by trying harder to sleep. You fix it by giving your nervous system the signals it needs to reset the curve. Most people see measurable change within 7 to 14 nights of consistent practice. Biology, not belief.*
Work With Your Biology Instead of Against It.
The Calm Sleep Reset is a complete 7-day protocol built on behavioral sleep science. Start with the free Calm Start Kit tonight, or go deeper with the full reset.
Sources & Further Reading
- Adam, E. K., Quinn, M. E., Tavernier, R., McQuillan, M. T., Dahlke, K. A., & Gilbert, K. E. (2017). Diurnal cortisol slopes and mental and physical health outcomes: A systematic review and meta-analysis. Psychoneuroendocrinology, 83, 25–41.
- Clow, A., Hucklebridge, F., Stalder, T., Evans, P., & Thorn, L. (2010). The cortisol awakening response: More than a measure of HPA axis function. Neuroscience & Biobehavioral Reviews, 35(1), 97–103.
- Hirotsu, C., Tufik, S., & Andersen, M. L. (2015). Interactions between sleep, stress, and metabolism: From physiological to pathological conditions. Sleep Science, 8(3), 143–152.
- Walker, M. (2017). Why We Sleep: Unlocking the Power of Sleep and Dreams. Scribner.
*Educational content only. Not medical, psychological, or therapeutic advice. Protocols shared for informational purposes. Consult healthcare professionals before making health changes. Individual results vary. References to research are for educational context; Better Life Habits does not claim clinical validation of its specific protocols.
